
Abductor hallucis tendinopathy causes heel pain on the bottom and inside of the heel which may radiate into the arch. This condition is very commonly misdiagnosed, often mistaken for plantar fasciitis heel pain because the two share the same origin at the heel, leading to similar symptoms when damaged.
What Is An Abductor Hallucis Strain?
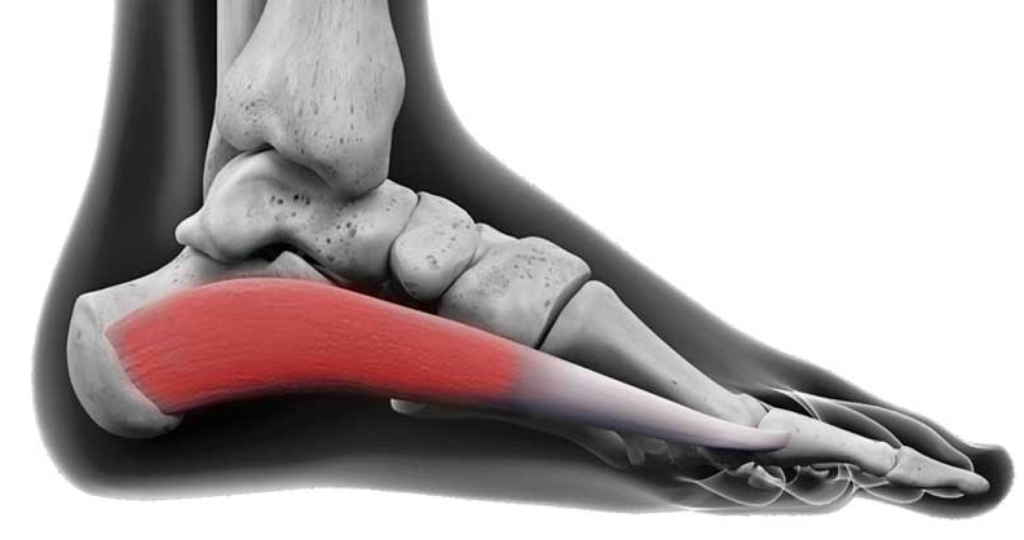 Your abductor hallucis is a muscle on the inside of your foot that literally means to abduct (move out away from the foot) the hallux (big toe). As such, this muscle helps to move your big toe out away from the other toes, like when you splay your toes out to grip onto the ground. It also plays an important function in stabilising the foot and arch and helping you take step after step.
Your abductor hallucis is a muscle on the inside of your foot that literally means to abduct (move out away from the foot) the hallux (big toe). As such, this muscle helps to move your big toe out away from the other toes, like when you splay your toes out to grip onto the ground. It also plays an important function in stabilising the foot and arch and helping you take step after step.
An abductor hallucis strain, or tendinopathy, describes damage to the abductor hallucis muscle or its tendon, which in most cases is caused by overuse – meaning that the abductor hallucis is overloaded and strained to the point of microtears in the tendon or muscle fibres. The body responds to this damage with symptoms of pain at the bottom and inside of the heel, swelling, pain radiating through the arch, pain that worsens first thing in the morning when getting out of bed, and pain that may be present even when rested. Some weakness in the muscle is also often noticed when trying to splay the toes.
The causes of the overuse and strain that our podiatrists see often include having a flat foot posture that increases the strain on the abductor hallucis with every step, wearing unsupportive shoes, increasing the intensity or duration of exercise suddenly and so ‘overdoing it’ on the day, working in a profession that involves lots of stair climbing, lifting heavy weights or gaining significant weight.
Can You Fix It?
Absolutely. Just like plantar fasciitis heel pain, treating abductor hallucis strains starts with reducing your current painful symptoms so you can feel more comfortable, and then working to help repair the abductor hallucis while putting the right measures in place to help prevent the problem from happening again.
How Do You Fix It?
All of our appointments include a comprehensive assessment by your podiatrist, including a video gait analysis and 3D foot scan. Paired with your history and getting to know your daily life and activities, we’ll be able to see the full picture about why this pain has developed for you. From here, we’ll discuss the best treatment approaches that are unique to you and your circumstances. These may include:
- Custom foot orthotics: orthoses will support the arch and reduce strain and tension on the abductor hallucis so it can begin to heal as opposed to being constantly stretched during activity. Orthotics will also address other abnormal foot biomechanics, including pronation, to optimise your recovery and help prevent future recurrence.
- Foot mobilisation: we may use foot mobilisation to address any stiffness, tension or dysfunction present in or around your foot and arch.
- Shockwave treatment: shockwave emits acoustic pressure waves to the heel and arch, directly over the abductor hallucis. This works to help reduce pain and inflammation, stimulate tendon regeneration, reboot the healing process in longstanding injuries, encourage the formation of new blood vessels, and more. You can learn about the benefits of shockwave treatment and why we love it here.
- Footwear review: we’ll assess your daily footwear to make sure it’s supporting your recovery (and your abductor hallucis) and not working against you.
- Strapping: strapping is a fantastic temporary way to immediately relieve stress on the abductor hallucis, thereby reducing pain and swelling.
- Stretching and strengthening program: once your initial pain and inflammation settle, using a targeted stretching and strengthening program will help to address tight or weak muscles that may be contributing to the development of your pain. Often, tight calf muscles encourage overloading of the inner foot, and so the calves are involved in the program.
- Activity modification: we may need you to modify certain movements or activities for a specific time to help offload the abductor hallucis and best support your recovery.
FAQs
What are the treatment options for Abductor Hallucis Tendinopathy?
Treatment options for Abductor Hallucis Tendinopathy focus on reducing inflammation, relieving pain, and healing the damaged muscle, while taking the right steps to help reduce the likelihood of the problems recurring in the future. The specific treatment plan may vary depending on the severity of the condition, but it may include a combination of the treatments we’ve specified above, paired with steps you can take at home such as resting and avoiding activities that aggravate the condition, applying ice packs to the affected area to reduce inflammation, and taking nonsteroidal anti-inflammatory drugs (NSAIDs) to alleviate pain and inflammation.
Can Abductor Hallucis Tendinopathy be prevented?
There are definitely measures you can take to reduce the risk of developing the condition or help prevent its recurrence. These include:
- Maintaining strong foot muscles through regular stretching and strengthening exercises.
- Wearing properly fitted footwear with adequate arch support and cushioning.
- Avoiding excessive or repetitive stress on the foot, such as overtraining or sudden increases in physical activity.
- Gradually increasing the intensity and duration of activities to allow the foot to adapt.
- Listening to your body and addressing any pain or discomfort promptly.
How long does it take to recover from Abductor Hallucis Tendinopathy?
The recovery time for Abductor Hallucis Tendinopathy can vary depending on the severity of the condition, the chosen treatment course, and individual factors. In mild cases, with appropriate treatment and rest, symptoms may improve within a few weeks. However, more severe or chronic cases may take several months for complete recovery. It’s important to follow the treatment plan recommended by your podiatrist, including rest, exercises, and any prescribed interventions.
Can I continue exercising or participating in sports with Abductor Hallucis Tendinopathy?
It’s important to allow sufficient rest and avoid activities that worsen the symptoms of Abductor Hallucis Tendinopathy during your initial stages of treatment. However, as your symptoms improve and with guidance from your podiatrist, you’ll be able to gradually reintroduce activities and exercises that do not cause pain or further damage. Modifying the intensity, duration, or type of exercise may be necessary to accommodate the healing process.
Can Abductor Hallucis Tendinopathy recur?
Yes, Abductor Hallucis Tendinopathy can recur, especially if the underlying causes or contributing factors are not addressed. Overuse, inadequate rest, improper footwear, and biomechanical abnormalities can increase the risk of recurrence. It’s important to follow the prescribed treatment plan, maintain foot strength and flexibility, and make necessary lifestyle modifications to reduce the risk of recurrence. If symptoms reappear, seeing your podiatrist can help prevent the condition from worsening.
Are there any specific exercises or stretches that can help with Abductor Hallucis Tendinopathy?
Yes, certain exercises and stretches can help with Abductor Hallucis Tendinopathy by strengthening the foot muscles, improving flexibility, and reducing stress on the affected tendon. Examples of exercises that may be beneficial include:
- Toe curls: Sit on a chair with your feet flat on the floor. Curl your toes to grip the floor and hold for a few seconds, then relax. Repeat this exercise several times.
- Towel scrunches: Place a towel on the floor and use your toes to scrunch it toward you. Repeat this motion several times.
- Calf stretches: Stand facing a wall, place your hands on the wall for support, and step one foot back. Keeping the back leg straight, bend the front knee and lean forward, feeling a stretch in the calf of the back leg. Hold for 20-30 seconds and repeat on the other side.
Can Abductor Hallucis Tendinopathy lead to other foot problems?
Abductor Hallucis Tendinopathy can sometimes contribute to other foot problems if left untreated or if the underlying causes are not addressed. It can lead to imbalances in foot mechanics, affecting the alignment and function of the foot. This, in turn, may increase the risk of developing conditions such as bunions, hammertoes, or plantar fasciitis. Timely diagnosis, appropriate treatment, and preventive measures can help minimise the risk of such complications.
Can I manage Abductor Hallucis Tendinopathy at home, or should I see a podiatrist?
While self-care measures, such as rest, ice, and over-the-counter pain relievers, may help alleviate mild symptoms of Abductor Hallucis Tendinopathy, it’s important to see a podiatrist for a proper diagnosis and treatment that will get you long-term results. A podiatrist can assess the extent of the condition, provide guidance on appropriate exercises and stretches, recommend specific footwear or orthotics, and consider which other interventions will be necessary.
