 Diabetes affects the circulation and feeling in your feet
Diabetes affects the circulation and feeling in your feet
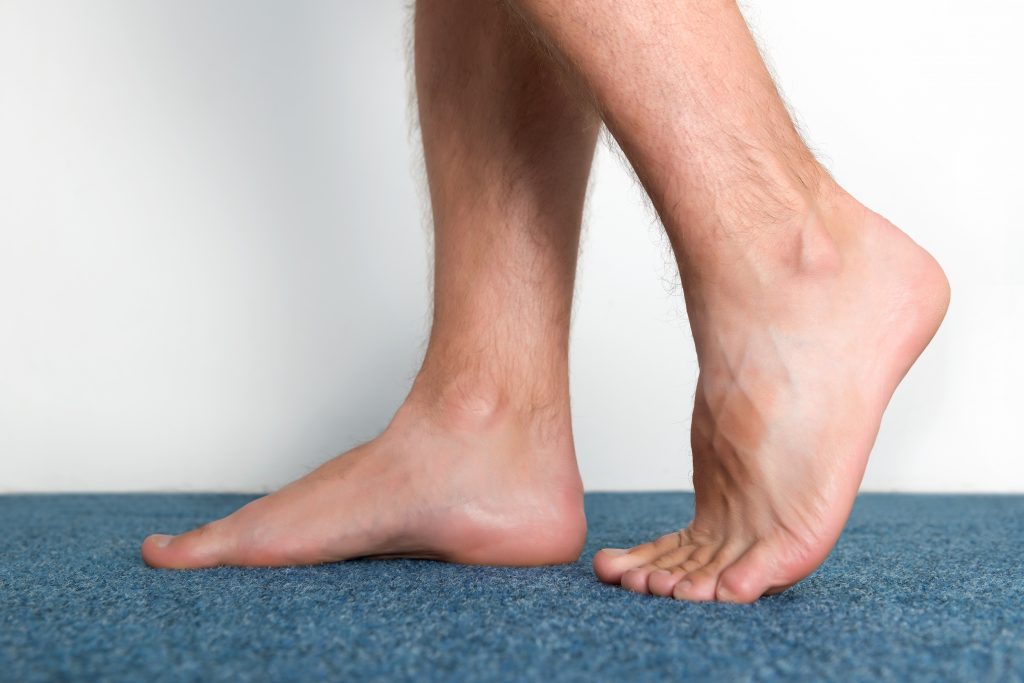
Diabetes can have a devastating impact on your feet because of the way it affects your sensation and your circulation. This means your ability to feel, and the blood flow to your feet.
These changes pose a serious risk for developing wounds, infections and ulcerations on the feet – which is why it’s so important to pay special attention to your feet. It’s also why a foot affected by diabetes is referred to as the ‘high-risk’ foot.
The symptoms you feel may start small, but will progressively worsen over time. This means that your foot care and advice must be specific to the symptoms you’re currently experiencing at this point time. This is why diabetic foot health checks are recommended annually, to keep you informed about how to best manage your foot health.
What are the symptoms of diabetes on your feet?
Over time, you may start to notice changes in circulation and sensation. These changes can then contribute to complications like ulcers.
Diabetes impairs your ability to feel (Peripheral Neuropathy)
Diabetes causes damage to the nerves in your feet and legs. As the nerves are responsible for our ability to feel, our ability to distinguish feelings may worsen, be mixed up, or may be lost altogether. This is called peripheral neuropathy, and can affect both the feet and hands. Symptoms include:
- Numbness
- Tingling
- Pins and needles
- Burning or pain
Ultimately, you may completely lose sensation in the feet. Unlike the blanket-like feeling of numbness, any feeling in the affected areas of the foot will be completely absent. This means you may not even realise that the sensation isn’t there. This is the most dangerous symptom as it renders you vulnerable to being unable to detect injuries like cuts or burns. If you can’t feel it, you don’t know you need to take action to treat and manage it. This injury may easily be something small like a pin, nail, or splinter. Any wound that results will be susceptible to infection, and if continued to be left untreated, the area may ulcerate.
Diabetes impairs your circulation
Diabetes also causes damage to the blood vessels, impairing the blood flow to the feet. Poorer blood supply to the feet means less oxygen and nutrients are delivered to a wound within a set timeframe. This means that the body will take longer to heal any cuts and breaks in the skin. If blood flow to the feet is impaired, you may experience:
- Cold feet
- Pale skin appearance
- Dry skin
- Brittle nails
When paired with an increased likelihood for undetected cuts and wounds from a diminished ability to feel, this is a very dangerous combination. It poses a significant risk of infection, ulceration, and at its worst, amputation. Diabetes is currently the leading cause of lower limb amputation, other than traumatic injuries.
What causes diabetes?
While type 1 diabetes is present at birth, type 2 diabetes can develop at any point throughout your life. It occurs when your cells become resistant to a hormone called insulin. Insulin works to direct sugar out of the bloodstream and into the cells. This means that sugar can build up in the bloodstream, damaging your vessels.
Managing diabetes at home
While diabetes requires a whole-body management plan, you can help manage the effects on your feet by:
- Checking your feet daily – look for cuts, blisters, bruises, colour changes, swelling and open sores. If you notice anything out of the ordinary, report it to your Podiatrist or GP immediately
- Using a mirror – to check the soles of your feet if you can’t see them otherwise
- Always protecting your feet – wear suitable footwear inside and outside your house, like slippers and sneakers
- Checking the inside your shoes regularly – for any sharp objects and rough edges that may pierce and damage the skin
- Washing your feet carefully – taking care to wash with antibacterial soap and drying well between the toes
- Applying moisturiser to feet daily – to help manage dry skin that may further reduce the sensation
- Cutting toenails straight across – and filing rough edges, to reduce the risk of piercing the other foot with sharp nails in bed
- Keeping wounds covered – with a dry non-stick dressing until you’re able to see your Podiatrist or PG
- Having your feet checked regularly by your podiatrist
How we can help
 Our podiatrists are qualified to help you manage the symptoms of diabetes on your feet, so you stay in control of your foot health. If you have diabetes, we recommend an annual assessment of your sensation and circulation, so you know the status of your foot health, and your risks. We give you advice and management strategies to help reduce the risk of complications and achieve the optimum outcomes for your feet.
Our podiatrists are qualified to help you manage the symptoms of diabetes on your feet, so you stay in control of your foot health. If you have diabetes, we recommend an annual assessment of your sensation and circulation, so you know the status of your foot health, and your risks. We give you advice and management strategies to help reduce the risk of complications and achieve the optimum outcomes for your feet.
During your assessment, we check every surface of your foot, including between the toes, to look for warning signs or changes from your last appointment. We’ll also help manage any wounds that develop. We may recommend diabetic-friendly footwear, and use devices like orthotics to help you feel more comfortable on your feet while reducing your injury risk.
Amputation prevention
Diabetic foot disease is the leading cause of lower limb amputation aside from accidents. The key to amputation prevention is early recognition and foot screening of those at risk. Those individuals considered to be at high risk are those who exhibit one or more of these six characteristics:
- Peripheral neuropathy, a nerve disorder generally characterised by loss of protective sensation and/or tingling and numbness in the feet Vascular insufficiency,
- A circulatory disorder which inhibits blood flow to the extremities
- Foot deformities, such as hammertoes
- Stiff joints
- Calluses on the soles of the feet
- A history of open sores on the feet (ulcerations), or a previous lower extremity amputation
Ready to take control of your foot health? Click here to book an appointment.
FAQs
How do I know if I have diabetes?
While a few signs and symptoms like extreme thirst, fatigue, hunger, slow-to-heal wounds and tingly sensations in the feet (among many more) may hint at the possibility of diabetes, the only way to know for sure is through blood and urine tests with your GP. Specifically, you may be asked to do a fasting blood glucose test, haemoglobin A1c test, and oral glucose tolerance test, and a urine analysis that looks for sugars. Always contact your GP if you’re concerned about diabetes for yourself or a loved one.
How can I check my feet if I can’t bend them up to see my soles?
Use a mirror – either place a mirror on the ground, or hold your foot up to a standing mirror. If you also have eyesight issues, it’s worthwhile to ask a family member or carer to check your feet at least once a week.
Do my risks differ depending on the type of diabetes I have?
No – type I and II diabetes both carry the risks of neuropathy and circulation issues. Your risk may be lower with gestational diabetes because it is typically a short-lived form of diabetes that is diagnosed in pregnancy and will go away after delivery. This means the exposure to higher blood sugars is fairly short-term, and many of the side effects do develop gradually over time. This does not mean you do not need to take extreme care if you have gestational diabetes – you absolutely do. Additionally, approximately half of all women who develop gestational diabetes will develop type II diabetes later in life.
I’ve been told I have pre-diabetes. What does this mean and what are my risks?
Pre-diabetes means that your blood sugar levels have been found to be higher than normal, but not enough to be clinically diagnosed with diabetes. It does mean that you have a higher risk of developing type II diabetes, alongside other serious health problems, including heart disease, and stroke. Without lifestyle changes to improve their health, 15% to 30% of people with prediabetes will develop type 2 diabetes within five years. Again, this means you need to take great care of your health and blood sugar levels to help you get the best outcomes for your health.
Is it true that you can’t play sports if you have diabetes?
Absolutely not. In fact, getting a healthy level of exercise is an important part of managing diabetes, with NZ guidelines recommending walking at least 30 minutes per day.
I’m concerned about the foot health of a parent with diabetes. Can I bring them in or do I need a referral?
Absolutely bring them in – while we accept all referrals from our GP colleagues, we do not require a referral for you to book in with us. Call us on 06 370 4057 to book an appointment.

