 Rheumatoid arthritis (RA) is an autoimmune disease, as opposed to the traditional ‘wear and tear’ arthritis (osteoarthritis). During a ‘flare’ or ‘episode’ of RA, your body’s immune system attacks the cells at the lining of your joints, producing painful symptoms. Rheumatoid arthritis can affect the whole body, primarily the small joints in the hands and feet, and is usually symmetrical.
Rheumatoid arthritis (RA) is an autoimmune disease, as opposed to the traditional ‘wear and tear’ arthritis (osteoarthritis). During a ‘flare’ or ‘episode’ of RA, your body’s immune system attacks the cells at the lining of your joints, producing painful symptoms. Rheumatoid arthritis can affect the whole body, primarily the small joints in the hands and feet, and is usually symmetrical.
What causes Rheumatoid Arthritis?
With Rheumatoid Arthritis, the body’s immune system attacks the joint capsule lining, called the synovial membrane. As the lining becomes inflamed, it can no longer produce the synovial fluid that lubricates the joints and nourishes the cartilage and bone ends. As a result, the joints stiffen and movement becomes harder. With repetitive inflammation after multiple flares, the cartilage and connective tissues become damaged, and the joint capsule can lose its ability to stabilise the joints.
While the exact reason for the body getting confused and attacking its own cells at the joints is not well understood, it has been thought that hereditary factors may increase your chance of developing it. Other contributing factors include smoking. Rheumatoid arthritis is more prevalent in women than in men.
Flares tend to begin without an identifiable cause, though some causes have been attributed to stress, illness and injury. Some of those affected report that cold temperatures and weather affects their symptoms.
What are the symptoms?
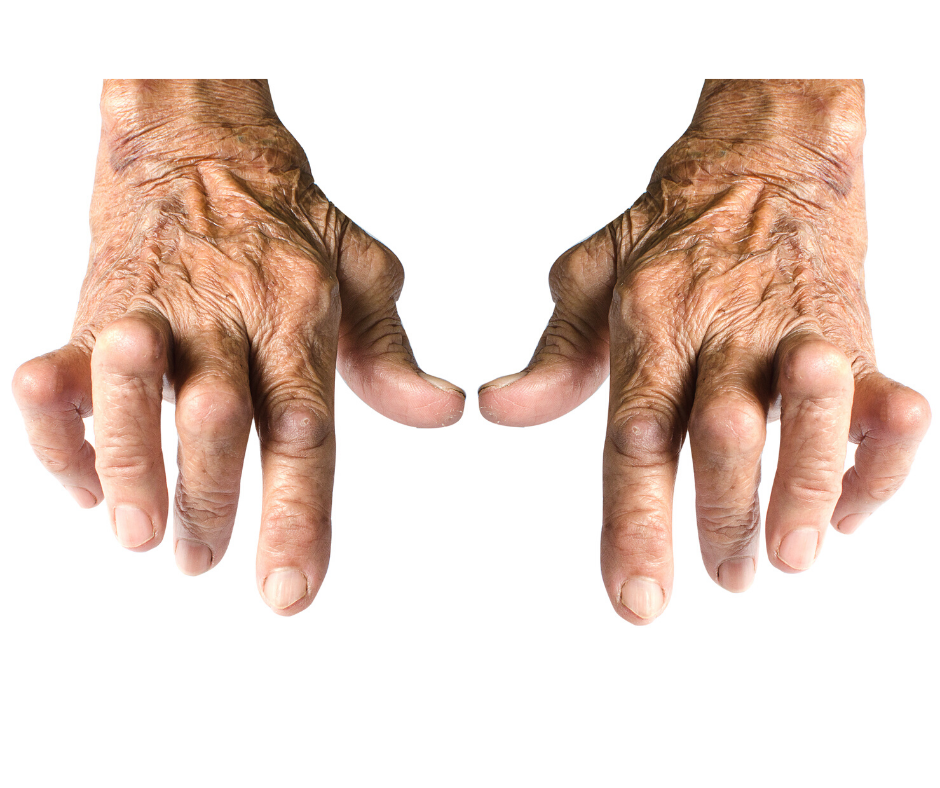 Symptoms of RA can include pain, swelling, and inflammation at the joints, stiffness or restricted movement, rheumatoid ‘nodules’, and changes to the shape of the joints over time.
Symptoms of RA can include pain, swelling, and inflammation at the joints, stiffness or restricted movement, rheumatoid ‘nodules’, and changes to the shape of the joints over time.
Can Rheumatoid Arthritis be treated?
While your GP may be able to provide medication to help manage and prevent your flares, as podiatrists here at Masterton Foot Clinic, we look at ways to reduce your pain, improve your comfort, and maximise your quality of life.
We often use custom orthotics to help increase your comfort, absorb shock from the forces when you hit the ground, and decrease the load through the high-pressure areas and joints of the feet. We also ensure that your footwear is assisting your comfort, and not holding you back. Prescribed exercises can help you maintain your muscle strength and range of motion at the joints, slowing down the progression of symptoms.
By keeping you moving comfortably, we hope to keep you independent, doing the things you love, and taking advantage of every opportunity.
FAQ’s
Can you help with rheumatoid pain and nodules in my hands?
Unfortunately we can’t. This is because we use non-medicated treatment approaches that are designed to make it more comfortable for you to walk and live with rheumatoid arthritis with regards to your mobility and foot and leg function. The hands are not our area of expertise and something that you should discuss with your doctor.
Can you do anything to help when a flare has already started?
Yes, when you’re having a painful flare in your feet, we can help by adding temporary padding or orthotics into your shoes to offload the inflamed joints, giving you some much-needed relief while you continue to walk.
Is there a cure for rheumatoid arthritis?
Rheumatoid arthritis is an incurable disease, but there are so many options available to help you manage this condition, minimise the symptoms, and live a healthy and active life. Medication is part of this, as is seeing a podiatrist, as well as working with a rheumatologist and other health professionals.
Is rheumatoid arthritis hereditary?
While it is not classed as a “hereditary disease”, research has shown that rheumatoid arthritis does have a genetic component. This means that if a parent has rheumatoid arthritis, your risk of having it is higher – though not guaranteed as the vast majority of people with rheumatoid arthritis have no immediate relatives (parents, siblings or children) that are affected by it.
Am I having a flare, or is it an injury?
Once you start having rheumatoid arthritis flares, the signs and symptoms will quickly become familiar. If you’ve recently been diagnosed then common signs include having symmetrical flares (on both sides of the body) that may affect one or more joints. You may also experience flu-like symptoms, your affected joints may become stiff, and you may experience pain and fatigue through your body.
