Plantar fasciitis describes an injury to a tissue called the plantar fascia at the bottom of your heel and foot. When the fascia is overloaded with pressure, is strained or is directly damaged, it becomes inflamed and tender. Your plantar fascia is a thick connective tissue band that originates from your heel and then spans your foot like a fan to connect to all five toes. You have connective tissues all around your body that work to connect, stabilise and enclose musculature and structures throughout the human body. Then plantar fascia helps to facilitate the function of the foot and maintain its shape, strength and flexibility. Not plantar fasciitis? While this is the most common cause of heel pain, other conditions like heel bursitis, stress fracture, growing pains in kids, Achilles problems, fat pad injury and other problems can also cause heel pain. During your first visit, you’ll receive a comprehensive assessment to confirm your diagnosis, and your condition will be explained. Plantar fasciitis is caused by overloading, overusing and straining the fascia past the point that it can handle so that micro-tears occur in the fibres of the tissue. This may be caused by: During resting or non-weight-bearing periods, the plantar fascia shortens. When body weight is rapidly applied to the foot the fascia must stretch and quickly lengthen, causing micro-tears in the fascia. Hypermobility, (excessive internal motion) of the foot can induce future or coexisting problems involving the knee, hip, sacroiliac joint or the low back region. Often, it is a combination of multiple causes that have ultimately overloaded the fascia. These causes must be corrected to prevent plantar fasciitis from being an ongoing problem for you in the future. The most common symptom of plantar fasciitis is heel pain first thing in the morning which tends to ease after a few minutes of walking. Other symptoms include: Symptoms can come and go over months or even years, without the problem being completely resolved. Because the damage to the fascia can worsen to a partial tear if left untreated, it’s important to see your Podiatrist to start your recovery. Care must also be taken as the symptoms of other conditions may also closely match the symptoms of plantar fasciitis. A good example of this is Abductor Hallucis Tendinopathy, where the Abductor Hallucis muscle shares an insertion at the base of the heel with the plantar fascia. After many years, a heel spur may develop on the bottom of the heel (calcaneus) in addition to plantar fasciitis. Having a heel spur, however, does not mean that you have or will develop heel pain. Heel spurs are visible on a lateral view x-ray of the foot. X-rays sometimes reveal very large heel spurs in patients that have never experienced any heel pain. It is not this bony spur, but rather the inflammation of the fascia that is attaching to the heel which causes discomfort. This is a common misconception. To learn more about heel spurs, see here. Once we understand exactly what has caused your plantar fasciitis, we will create a comprehensive treatment plan for you that takes into consideration your daily activities, lifestyle and goals. Initially, the focus of the treatment plan will be to reduce your current symptoms and get you out of pain, while long-term your treatment plan will work to prevent this from happening again. Once you’ve had plantar fasciitis, you’re more likely to damage your fascia again, so future prevention is important. Depending on the severity of your symptoms, your treatment may include: Just like you can break your leg or sprain your ankle twice, you can definitely develop plantar fasciitis again. The key is to have the right preventative measures in place to reduce the risk of this happening again. By knowing about the condition and its causes, you can make the best decisions for your feet. Make sure you talk through any questions you have with us so you can understand how to best protect and look after your feet. https://www.mastertonfootclinic.co.nz/heel-spurs/
Plantar fasciitis is the largest cause of heel pain that we treat.

What causes plantar fasciitis?
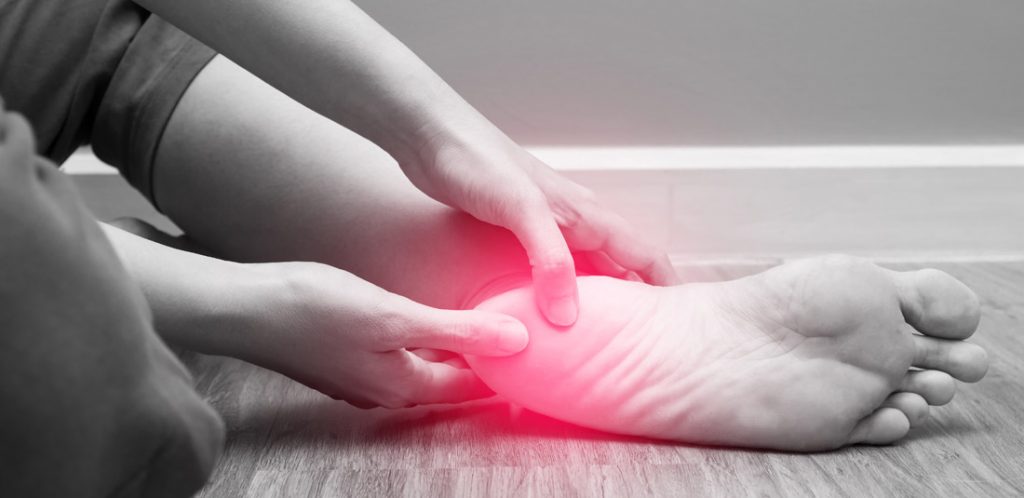 Symptoms
Symptoms
Heel Spurs
How is plantar fasciitis treated?
Will the pain come back?
FAQs
Are plantar fasciitis and a heel spur the same thing?
The term ‘plantar fasciitis heel pain’ and a heel spur are often used interchangeably – even by other health professionals. But in reality, they are two very different things. A heel spur means that there is a prominence – a spur – protruding from the heel bone. This is usually some calcification (hardening) at the tendon that attaches to the heel. On the other hand, plantar fasciitis means that a tissue called the plantar fascia, which starts at the bottom of the heel and fans out to attach to the toes, has become damaged or irritated.
Isn’t a heel spur a bone spike – how can you fix it without surgery?
Two ways – first by remembering that, as we described above, when most people say that they have a heel spur, they really have plantar fasciitis, which is tissue damage. Where a heel spur is present, it actually may or may not be causing symptoms, as research has demonstrated that many people with a heel spur feel no heel pain, and many people with heel pain display no heel spur. Where a heel spur is causing problems, however, we use shockwave which can help break down tendon calcifications.
Why are orthotics recommended for heel pain?
Heel pain can have a wide variety of causes, and many of them are linked to foot posture and biomechanical foot function (the way your feet and legs work together to produce movement). Many times, it is dysfunctional movement patterns or poor foot posture that is a big issue. Custom foot orthotics work to adjust how the feet are positioned and move, and therefore can unload the tissues and structures that are being overloaded when heel pain is present. Hence, they are recommended not only as part of your treatment, but also for future prevention.
We should note that – not everyone will need orthotics for their foot pain or problem. Orthotics should only be recommended and prescribed after a thorough assessment with your podiatrist, who will confirm that orthotics can help. Not everyone needs orthotics.
Why do you offer a specialised heel pain rehab program?
We offer the Happy Heel treatment because we see hundreds of people with heel pain every year, and over the years, we have really refined what works best for our patients. We developed our proven process for heel pain both from evaluating the research and evidence, which involved us incorporating new and innovative treatments like shockwave therapy and making it available in our clinic, and understanding what is working best for our local Masterton residents in terms of their lifestyle and quality of life. The result is a specialised rehab program that has similar foundations but is personalised for each individual based on their symptoms and the results of their assessment.
Will my heel pain go away on its own?
Heel pain can go away on its own, but it is much less likely than other areas of your body. That’s because, with heel pain, the damaged structures are constantly being used and loaded every time we walk or stand – so they never get a break long enough to truly heal. Moreover, if we have a tough or long day on our feet, we may even worsen our heel pain by placing more strain on it than it can handle in its damaged and vulnerable state.
Is heel pain related to back pain?
It may be. Some studies have shown that up to 75% of people with ongoing heel pain are shown to have unmanaged low back pain or low back dysfunction. Of course, this all depends on the cause of both the heel pain and back pain respectively. Heel pain can occur as a result of sciatica in the back, or from problems in the spine like a herniated disc. Other times, it may be a dysfunctional movement pattern that is adding extra strain on both your back and your feet and legs. It can also be possible that your back pain is independent of whether or not you have heel pain and vice versa.
How can I strap my foot if I have heel pain?
We’ve demonstrated a strapping technique for you here.
Can heel pain cause knee pain?
Yes it can. For some people, when they’re experiencing heel pain, they may change the way they walk to try to protect the heels and avoid movements that cause pain. This abnormal and altered gait pattern may then place excess strain on the knees and lead to knee pain.
Why does heel pain start out of the blue?
It’s likely that your heel pain hasn’t started completely out of the blue, but your movement patterns or foot posture has been leading to this for some time, with a certain day being the ‘breaking point’ where symptoms started. When it does happen out of the blue, it may be the particular activity you did that day – like going on a long hike – that placed more strain on your heels than they could handle without damage.
Can heel pain be prevented?
Yes! Heel pain can be prevented by understanding what’s causing it, and then addressing the causes. For some, this may look like wearing supportive sneakers instead of their jandals. For others, it may be stretching their Achilles tendon and strengthening their legs. For others, it may be helping correct their poor foot posture using custom foot orthotics.
Is heel pain genetic?
You can inherit factors that increase your likelihood of heel pain, like having flat feet. But just because your family had heel pain, doesn’t mean that you will – especially if you address and treat the factors that put you at risk.
Is heel pain covered by health insurance?
This is dependent entirely on your policy and level of cover. If your policy covers podiatry, then it is likely your insurer will be able to assist. Please contact your insurer directly to confirm.
Is heel pain covered by ACC?
If your heel pain is a result of an accident, then you may be eligible for ACC. We can fill in a claim form for you and submit it to ACC, who will ultimately decide if your injury is covered.
How does foot mobilisation work for heel pain?
Foot mobilisation works by breaking down scar tissue, helping better lubricate the joints in the feet, and relieving pain. When used for heel pain, the feet are manipulated to improve the alignment of the joints, release tension and help the feet and legs function more efficiently. Ultimately, when combined with our other components of the heel pain treatment, this helps you get out of pain and get your feet moving better to reduce the risk of your heel pain recurring.
