
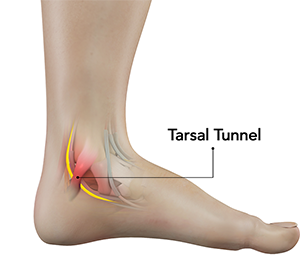
Tarsal tunnel syndrome produces pain, numbness, tingling or burning sensations on the bottom of the foot, often around the heel. It occurs when a prominent nerve (the posterior tibial nerve) is compressed when it passes through a dedicated space near the inside of the ankle called the tarsal tunnel, named after the tarsal bones of the foot where the tunnel is located.
 The symptoms of tarsal tunnel syndrome are produced when there is pressure on the nerve. This pressure can be caused by a multitude of things, including:
The symptoms of tarsal tunnel syndrome are produced when there is pressure on the nerve. This pressure can be caused by a multitude of things, including:
- A flat foot posture which can lead to the nerve being stretched or compressed over time
- Soft tissue masses in the area of the tunnel such as cysts, fibromas, ganglions or lipomas, which then press on and compress the nerve
- The development of small varicose veins around the nerve that can cause compression
- A foot or ankle injury that leads to swelling in the area that compresses the nerve
- Sports and sports-related injuries that place high demands on the foot and ankle and can lead to damage and swelling
- Inflammatory conditions
Diagnosing Tarsal Tunnel Syndrome
Diagnosing tarsal tunnel syndrome starts with your medical history, injury history and a clinical exam to understand which movements compress the nerve and produce your symptoms. For those whose symptoms are a result of their foot posture, we often find the symptoms are easily reproduced by moving the foot outwards which stretches the nerve, and the symptoms resolve when we turn the foot to face it inwards, which creates more of an ‘arched’ foot shape. Where the cause is unable to be determined clinically, we may refer you for an x-ray or ultrasound to look for any masses like cysts that may be present in or near the tunnel.
Treatment
Treating tarsal tunnel syndrome must be directed at the cause of the impingement. Before you’re able to get in to see your podiatrist, avoid any movements that bring on your painful symptoms as these can lead to further irritation and swelling, which may worsen your symptoms. It’s a good idea to take notes of exactly which movements and positions produce symptoms, as this will give valuable information to your podiatrist to use in their assessment.
If your foot posture is the cause of your symptoms, whether that’s from flat feet or other movement dysfunction, we may recommend treatments like custom foot orthotics to adjust the alignment of your feet and your foot biomechanics, or foot mobilisation therapy to help free up the joints in your feet to move without restriction (and therefore ease the potential strain on the tarsal tunnel).
If your nerve impingement is caused by a mass in the tarsal tunnel, we’ll assess this on a case-by-case basis, examining what the mass is and how best to help manage it and any specialists to involve in your care.
Frequently Asked Questions
Can tarsal tunnel syndrome lead to long-term complications?
Yes – unfortunately without proper treatment, tarsal tunnel syndrome can result in chronic pain, muscle weakness, and sensory changes in the affected foot.
Is tarsal tunnel syndrome more common in athletes?
Tarsal tunnel syndrome affects people of all ranges of activity levels, not just athletes. With that said, as repetitive movements and overuse can contribute to its development, we definitely see a fair few cases of tarsal tunnel in those that like to stay physically active – including just taking long evening or weekend walks.
Can tarsal tunnel syndrome occur on both feet simultaneously?
Yes, tarsal tunnel syndrome can affect one or both feet, depending on the underlying causes and contributing factors. With that said, we usually only see one foot affected at a time.
Is tarsal tunnel syndrome more common in certain age groups?
Tarsal tunnel syndrome can occur in individuals of all age groups, but it is more common in adults and older individuals, especially those with underlying health conditions that affect nerve health.
