Gout is an inflammatory arthritis that occurs when uric acid builds up in a high concentration in the blood.
Uric acid is a by-product of purines, which are chemicals that are naturally found in our food. Uric acid may build up because the kidneys have difficulty processing the acid at a regular rate, or because our diet contains too much food that is purine-rich, like red meat, shellfish, red wine and beer.
When uric acid is present in high concentrations in the blood, it can crystallise, causing severe pain and discomfort. For 90% of people, these crystals will develop at either the big toe joint or other joints in the feet. This location in the feet occurs because cooler temperatures promote crystallisation, and our feet are often one of the coolest partest of our bodies.
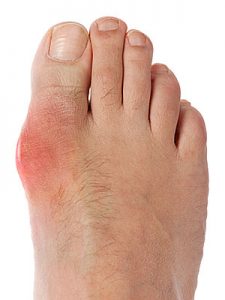
What does gout feel like?
When the uric acid crystallises, this is known as an ‘attack’ or ‘flare-up’ of gout. You’ll feel sharp pain that can come on suddenly, and the joint may feel warm, red and swollen.
Are you more likely to develop gout?
Gout can affect anyone at any time, but often affects men between the ages of 30 and 60.
If one of your family members has had gout, you are more likely to develop it too, so should be careful about consuming food that has excess purine levels. Other contributing factors may include aspirin, diuretics, stress, high blood pressure, surgery and diabetes.
How is gout treated?
The first step to managing gout is to ensure that a high level of uric acid is causing your symptoms with a blood test. This will rule out other causes of damage to the joints causing your pain.
Aside from reducing your intake of purine-rich foods, we recommend helping wearing warm socks and keeping your feet warm to help prevent crystallisation. Staying active and exercising (when you don’t have a flare) will help manage other factors that contribute to gout such as obesity, stress and diabetes.
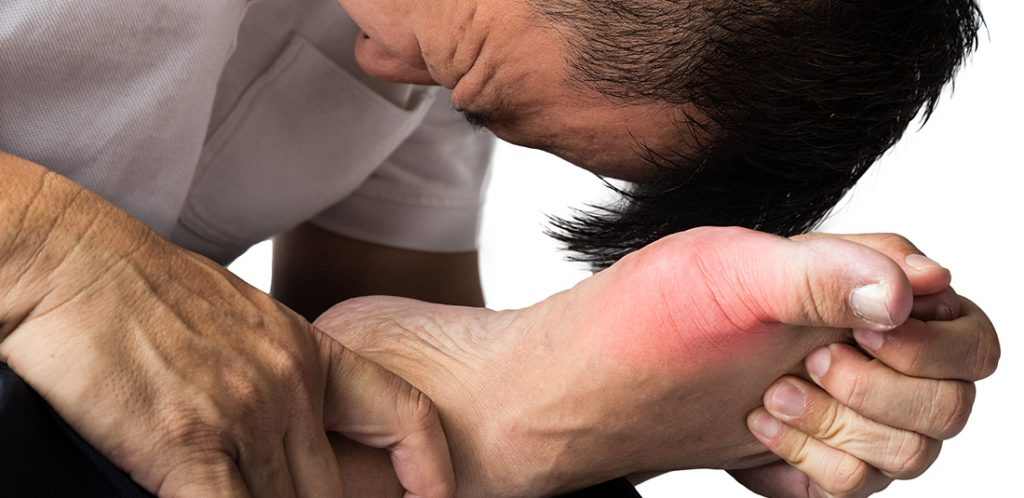
During a flare, try to avoid adding additional pressure to the affected joints. Wear comfortable shoes that help you feel better, and don’t put more weight on the affected joints.
We often help out patients with gout by conducting a comprehensive biomechanical examination of your feet and legs, looking for any musculoskeletal factors that may be contributing to your pain. If suitable, we may use comfortable custom orthotics to help relieve painful symptoms that occur due to restrictions in the mobility of your feet.
FAQ’s
Can you diagnose gout?
Our podiatrists can indicate whether the joint flare you’re experiencing may be gout, but you will need to have your condition formally diagnosed by your doctor with laboratory testing. This may include a blood sample, or a sample of the fluid from the affected joint if you are currently having a flare.
Will wearing warm socks help prevent gout?
It is thought that uric acid crystallises in cooler temperatures, so there is merit to the idea that wearing warm socks may help prevent a gout flare. We also recommend regular exercise as it helps promote circulation and body temperature.
Does gout usually appear in the same joint each time?
Most often, but not always. Typically, gout only affects one joint at a time, and it tends to be the big toe joint. For some people, the lesser toes, ankle or knee may be affected. From the patients we see, they tend to have the same joint affected each time.
How long does a gout flare last?
If you’re on medication, then your flare may pass as quickly as within 3 days. Without medication, this may be closer to two weeks.
What is pseudogout?
Pseudogout is also a type of arthritis that presents with similar signs and symptoms as gout including joint flares. The difference is that while gout is caused by uric acid crystals in a joint, pseudogout is caused by calcium phosphate crystals.
Is gout hereditary?
While gout is not a formal hereditary disease, there is some genetic link, according to research. That means if parents have gout, the children have a higher risk of developing it, though this doesn’t mean they will. Many causes of gout are attributed to lifestyle and food intake.
What’s my outlook with gout?
Most of the patients we see with gout are able to live active and independent lives without being restricted by their gout. Both medical management and optimising their foot comfort and function with the help of our podiatry team goes a long way. There are also many modifiable risk factors that you can address to reduce your gout flare occurrence.
